The modern conversation about longevity has changed significantly over the past decade. Longevity is no longer just about increasing lifespan, the total years a person lives, but about enhancing healthspan, the years during which a person stays vibrant, cognitively sharp, metabolically resilient, and physically able.
For clinicians, particularly chiropractors practicing within a functional or integrative model, this shift presents an opportunity. Longevity medicine is no longer confined to anti-aging clinics or elite biohacking communities. It has become a clinically relevant framework for addressing chronic inflammation, neurodegeneration, metabolic dysfunction, and immune dysregulation.
At the center of this emerging model are three deeply interconnected physiological systems:
- The gut–brain axis
- Mitochondrial bioenergetics
- Cellular signaling pathways governing inflammation and repair
When these systems communicate efficiently, the body maintains resilience. When they break down, accelerated biological aging and chronic disease often follow.
A growing body of research and clinical applications suggests that combining functional medicine diagnostics, targeted lifestyle strategies, and non-thermal low-level laser therapy (LLLT) may provide a powerful framework for restoring cellular communication and improving patient outcomes.
This article explores five core pillars of longevity medicine and how clinicians can translate them into practical clinical strategies.
⏱ Healthspan vs Lifespan: Redefining the Longevity Model
For most of the 20th century, longevity research mainly aimed to extend lifespan. However, living longer doesn’t always mean living better. Today, healthspan is a more meaningful measure. Healthspan signifies the portion of life lived without debilitating chronic illness—where functional mobility, metabolic efficiency, cognitive clarity, and immune resilience are preserved.
Increasing evidence shows that biological age, rather than chronological age, is a more accurate predictor of disease risk and mortality. Biological age reflects the cumulative effects of mitochondrial efficiency, muscle mass and strength, hormonal balance, inflammatory load, nutrient signaling pathways, and lifestyle patterns.
One of the strongest indicators of biological aging is skeletal muscle mass. Muscle tissue acts as a metabolic organ, affecting glucose disposal, insulin sensitivity, inflammatory signaling, and immune function.
Sarcopenia, the loss of muscle mass, is closely linked to issues such as cardiovascular disease, cognitive decline, frailty, falls, and metabolic syndrome. Hormonal signaling significantly influences this process, with decreases in testosterone, growth hormone, and DHEA, as well as reduced insulin sensitivity, affecting mitochondrial function and the body’s ability to repair tissues.
Lifestyle interventions that boost healthspan include resistance training, optimizing sleep, aligning circadian rhythms, following nutrient-dense diets, and managing stress. These approaches primarily operate at the cellular level by improving mitochondrial function and supporting metabolic signaling pathways.
🧠 Gut-Brain Axis & Neuroinflammation
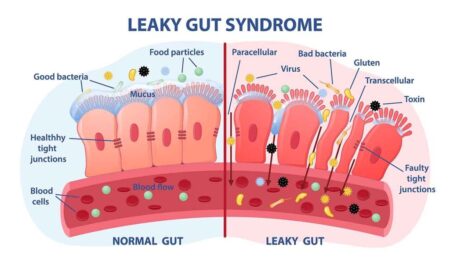 A breakthrough in modern physiology is the recognition of the bidirectional gut–brain axis, a communication network in which the gut and brain interact through multiple interconnected systems, including the vagus nerve, immune signals, microbial metabolites, neurotransmitters, and hormones.
A breakthrough in modern physiology is the recognition of the bidirectional gut–brain axis, a communication network in which the gut and brain interact through multiple interconnected systems, including the vagus nerve, immune signals, microbial metabolites, neurotransmitters, and hormones.
Disruptions in this communication network are now closely linked to various chronic illnesses such as Alzheimer’s, Parkinson’s, depression, anxiety, autoimmune conditions, and metabolic syndrome.
A key factor in gut–brain issues is intestinal permeability, commonly known as “leaky gut.” When the gut barrier is damaged, endotoxins, such as lipopolysaccharides (LPS), can leak into the bloodstream. This causes widespread immune activation and persistent inflammation, which can lead to neuroinflammation. Such neuroinflammation may impair synaptic communication, disrupt mitochondrial function, and affect cognitive abilities.
The microbiome also plays a crucial role. Gut bacteria generate metabolites like short-chain fatty acids (SCFAs), serotonin precursors, gamma-aminobutyric acid (GABA), and dopamine intermediates that affect brain function. An imbalance, or dysbiosis, in the microbiome can disrupt neurotransmitter levels and immune system regulation.
Clinical assessment strategies may include:
- Comprehensive stool analysis
- Microbiome sequencing
- Intestinal permeability markers
- Inflammatory cytokine testing
Correction strategies often involve:
- Anti-inflammatory nutrition protocols
- Targeted probiotic and prebiotic interventions
- Polyphenol-rich foods
- Stress and vagal tone optimization
Restoring communication between the gut and the brain can significantly reduce overall inflammation and enhance cognitive resilience.
⚡ Mitochondrial Dysfunction & the Electron Transport Chain
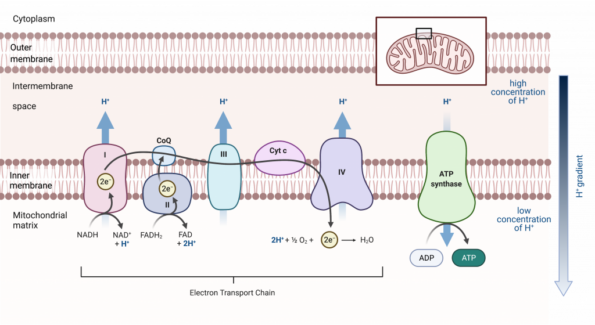 At the cellular level, longevity is mainly a bioenergetic process. Mitochondria generate most of the body’s ATP via a biochemical system called the electron transport chain (ETC).
At the cellular level, longevity is mainly a bioenergetic process. Mitochondria generate most of the body’s ATP via a biochemical system called the electron transport chain (ETC).
The ETC is made up of four core protein complexes located in the inner mitochondrial membrane.
- Complex I
- Complex II
- Complex III
- Complex IV
Electrons from nutrient metabolism pass through these complexes, creating the electrochemical gradient needed for ATP production. However, mitochondrial efficiency decreases with age and chronic disease. Contributing factors include oxidative stress, persistent inflammation, environmental toxins, nutrient deficiencies, a sedentary lifestyle, and microbial metabolites from gut dysbiosis, all of which impair mitochondrial function.
When mitochondrial complexes are disrupted, electrons escape from the electron transport chain, leading to the generation of reactive oxygen species (ROS). Although ROS serves signaling functions in healthy cells, excessive amounts can harm cellular membranes, DNA, proteins, and mitochondrial enzymes. This damage speeds up biological aging and plays a role in conditions like Alzheimer’s, Parkinson’s, cardiovascular disease, diabetes, and chronic fatigue syndrome.
Strategies to restore mitochondrial function typically aim to increase mitochondrial biogenesis, sustain redox balance, and improve ETC efficiency. Key nutritional approaches involve compounds such as coenzyme Q10, alpha-lipoic acid, acetyl-L-carnitine, magnesium, and polyphenols. Recent studies also suggest that non-thermal LLLT can directly stimulate mitochondrial complexes.
💡 Laser-Based Functional Medicine for Cellular Optimization
 Non-thermal LLLT is one of the most promising new techniques for optimizing cellular function. Unlike surgical lasers, LLLT employs low-intensity, non-thermal light wavelengths to activate biological processes within cells.
Non-thermal LLLT is one of the most promising new techniques for optimizing cellular function. Unlike surgical lasers, LLLT employs low-intensity, non-thermal light wavelengths to activate biological processes within cells.
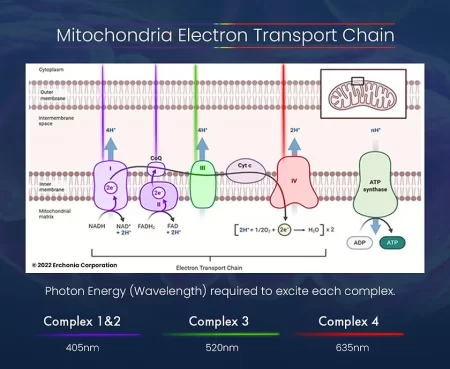
Research suggests that specific wavelengths of visible light interact with distinct components of the mitochondrial electron transport chain (ETC), influencing cellular energy production. Red light at approximately 635 nm interacts with cytochrome c oxidase, the terminal enzyme of Complex IV, facilitating more efficient electron transfer and supporting mitochondrial respiration. Shorter wavelengths appear to influence earlier portions of the ETC. Violet light (405 nm) is associated with activity in Complexes I and II, while green light (520 nm) influences Complex III.
When these wavelengths stimulate their respective mitochondrial targets, the result can be enhanced electron transport efficiency, improved mitochondrial membrane potential, and increased adenosine triphosphate (ATP) production. These effects may contribute to improved cellular energy output, better regulation of oxidative stress, enhanced tissue repair signaling, and greater overall metabolic resilience.
LLLT may also modulate nitric oxide signaling, thereby enhancing microcirculation and tissue oxygenation. These mechanisms make LLLT especially relevant for conditions involving mitochondrial dysfunction and inflammation, such as neurodegenerative disorders, chronic musculoskeletal pain, peripheral neuropathy, cognitive decline, and immune dysregulation.
From a functional medicine viewpoint, laser therapy provides several benefits:
- Non-pharmacologic
- Minimal side effects
- Compatible with nutritional and lifestyle interventions
- Capable of targeting specific tissues and physiological systems
When incorporated thoughtfully into a comprehensive clinical approach, laser-based therapies can improve mitochondrial function and accelerate tissue healing.
📋 Actionable Longevity Protocols & Clinical Algorithms
The main aim of longevity medicine is to translate knowledge into practice, not just to acquire theoretical understanding. Practitioners must move seamlessly from concepts to practical applications by implementing structured protocols. A useful longevity care framework could consist of three phases of care.
1. Acute Phase: Stabilization & Inflammation Reduction
The main goal is to reduce inflammation and restore essential physiological functions. Key strategies might include:
- Anti-inflammatory nutrition protocols
- Gut barrier repair strategies
- Targeted microbiome restoration
- Vagal nerve stimulation techniques
- Low-level laser therapy applied to affected tissues
Laser frequency during this phase might need several sessions per week, especially for patients with significant inflammation or neurological symptoms.
2. Chronic Phase: Cellular Restoration
Once acute inflammation is stabilized, the focus shifts to mitochondrial repair and metabolic optimization.
Interventions may include:
- Mitochondrial nutrient protocols
- Resistance training programs
- Sleep and circadian rhythm optimization
- Hormonal evaluation, where appropriate
- Laser therapy targeting mitochondrial stimulation and tissue repair
This phase typically takes several months of consistent intervention to restore metabolic resilience.
3. Wellness Phase: Healthspan Optimization
Once cellular function stabilizes, patients can move into long-term longevity strategies. Goals during this phase include:
- Preserving muscle mass
- Maintaining metabolic flexibility
- Supporting microbiome diversity
- Optimizing mitochondrial efficiency
Laser therapy might be applied periodically during this phase to aid recovery, enhance circulation, and promote cellular function.
The Future of Longevity Medicine
Longevity science is progressing rapidly, but certain fundamental principles are becoming clearer. Achieving true longevity does not rely on a single intervention; rather, it depends on the coordinated enhancement of cellular communication systems, including gut–brain signaling, immune regulation, mitochondrial function, and redox balance. When these systems work together harmoniously, the body can better resist aging and disease. For practitioners in integrative or functional medicine, this offers a significant and promising opportunity.
By incorporating advanced diagnostics, lifestyle medicine, targeted nutrition, and cutting-edge technologies like non-thermal low-level laser therapy, practitioners move beyond symptom management towards genuine physiological restoration. The future of healthcare isn’t just about prolonging life; it’s about enhancing vitality, cognitive function, and cellular resilience throughout a person’s entire lifespan. This future starts with restoring communication at the most fundamental level of human physiology – the cell.
Inspired by what you’ve read? Experience it Live
Dr. Robert Silverman will be in Australia this May, presenting at two exclusive events designed to help clinicians translate longevity science into real-world practice. If the ideas explored in this article sparked new possibilities for your practice, this is your opportunity to take them further.
Join us on the Gold Coast and be part of the clinicians leading the evolution of healthcare.

Integrative Aesthetics Reset
Body Contouring & Wellness Program
Integrative Aesthetics Reset is a focused one-day educational workshop examining a modern, integrative approach to fat loss, metabolic health and wellness. The program supports cross-disciplinary care across aesthetics, wellness, nutrition and functional practice, reflecting the growing need for clinics to integrate clinically, ethically and practically.

Integrative Practice Summit
Longevity & Healthspan Intensive Program
Integrative Practice Summit is a comprehensive two-day educational workshop exploring the science of longevity, healthspan and whole-system clinical care to support recovery, resilience and long-term function. The program supports cross-disciplinary care across medical and allied health professions.